Author: dr. Aisha Savannah
Supervisor: dr. Indah Purnamasari, Sp.DVE, M.Ked.Klin
Port-wine stain (nevus flammeus), also known as congenital capillary malformation, is a non-neoplastic congenital dermal capillary vascular malformation that presents as a pink to port-wine-colored patches or red macular patch on skin since newborn and persists throughout life. It results from differentiation-impaired endothelial cells (ECs) in human skin, leading to the progressive dilatation of immature venule-like vasculature.1
The prevalence of PWSs is estimated to range from three to five cases per 1,000 live births. Approximately 1.2 million individuals in the United States and around 26 million people worldwide are affected by PWSs birthmarks. There is no observed sex predilection, and the condition typically occurs sporadically rather than following a hereditary pattern. In rare cases, PWSs may be acquired during adolescence or adulthood and their development may be related to trauma to the affected skin.1,2
Port-wine stains (PWSs) appear as well-defined patches that may be unilateral, bilateral, or centrally located, typically exhibiting a pink or red coloration. PWSs on the face commonly manifest in areas innervated by the trigeminal nerve (dermatomes V1 and V2). These lesions are characterized by structural abnormalities in the intradermal capillaries. While PWSs can occur on any part of the body, the oral mucosa is not exempt from their development. Sometimes the patches may darken, thicken, and develop nodules over time.1 Clinical manifestation of PWS can be seen in Figure 1.3
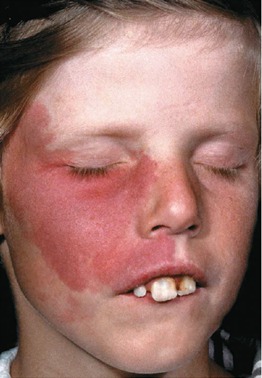
Source: Wolff K, Johnson RA, Saavedra AP. Fitzpatrick dermatology flashcard.
New York: Mc Graw Hill Education. 2014. p.70.
Several therapeutic approaches have been used in the management of port-wine stains (PWSs), including tattooing, cryosurgery, ionizing radiation, CO₂ laser therapy, and electrotherapy. However, these modalities generally demonstrated low efficacy and were frequently associated with considerable adverse effects. Currently, pulsed dye laser (PDL) therapy with wavelengths of 577, 585, and 595 nm is widely recognized as the gold standard for the treatment of PWSs. In addition to PDL, alternative treatment modalities have been investigated, including topical antiangiogenic agents and other laser-based technologies such as intense pulsed light (IPL), small and large spot 532 nm potassium-titanyl-phosphate (KTP) laser, 1064 nm neodymium-doped yttrium aluminum garnet (Nd:YAG) laser, and the 755 nm Alexandrite laser.4,5
The therapeutic mechanism of these laser systems relies on the principle of selective photothermolysis, in which laser energy is preferentially absorbed by vascular chromophores within the lesion, particularly oxyhemoglobin, deoxyhemoglobin, and methemoglobin. Absorption of this energy results in localized heat generation that induces vascular damage while minimizing injury to adjacent tissues. Early initiation of laser therapy, particularly during infancy, is considered important to achieve more favorable treatment outcomes. Nevertheless, a considerable proportion of patients may still experience suboptimal responses, indicating the need for additional or alternative treatment strategies.6
Photodynamic therapy (PDT) has also been reported as a safe and effective therapeutic option for facial PWS in pediatric patients. Moreover, the large-spot 532 nm KTP laser has shown promising efficacy in the treatment of PWS lesions located on the body.4,7 A study conducted by Siskawati (2024) demonstrated that treatment initiated during the macular or early stage of PWS may help prevent progression to hypertrophic or nodular lesions. Furthermore, repeated sessions of 577-nm vascular laser therapy have been shown to slow disease progression and produce significant clinical improvement.4
Quality of Life and Psychological Effects on PWSs
Port-wine stains (PWS) located on the facial region may result in noticeable cosmetic disfigurement and can contribute to social stigma. These vascular lesions often become more pronounced with increasing age, which may further complicate social interaction and adaptation, particularly during childhood. As a result, children with PWS are frequently subjected to discrimination or negative responses from their peers.1
A study conducted among school-aged children with visible facial differences—including PWS, burn scars, infantile hemangiomas, and congenital melanocytic nevi—demonstrated a reduced quality of life and impaired psychological well-being when compared with healthy peers. Interestingly, these psychosocial effects were not observed in preschool-aged children. Parents often face a difficult decision when considering treatment, as they must balance the potential long-term social consequences of untreated PWS with the discomfort, procedural pain, and financial burden associated with laser therapy.8,9
Hagen et al. (2017) reported that facial PWS has a significant negative impact on patients’ quality of life. Adolescents and adults with PWS experienced more pronounced social difficulties compared with younger children. In addition, adult patients frequently reported dissatisfaction with how they were perceived and treated by others. Many also believed that the presence of the skin condition negatively affected their ability to establish romantic or sexual relationships.9
Similarly, a recent study by Lipinska et al. (2025) demonstrated that PWS significantly affects patients’ psychosocial well-being, including overall quality of life, body image perception, and feelings of stigmatization. In this study, 59 adult patients completed an online survey that included several validated psychological assessment tools, such as the Dermatology Life Quality Index (DLQI), Skindex-29, Perceived Stigmatization Questionnaire (PSQ), Dysmorphic Concern Questionnaire (DCQ), and Hospital Anxiety and Depression Scale (HADS). Based on DLQI results, a decreased quality of life was reported in 52.5% of participants. Furthermore, HADS analysis revealed symptoms of anxiety in 45.8% of patients and depression in 22%. Findings from Skindex-29 indicated that PWS had a moderate negative impact on patients’ daily lives, while DCQ results suggested that more than half of the participants experienced disturbances in body image perception.10
In a conclusion, the management of patients with PWS requires holistic approach. Early diagnosis and intervention, combined with appropriate therapeutic strategies, psychological support, and continuous patient counseling are essential for improving clinical outcomes and overall quality of life. Through a multidisciplinary and patient-centered approach, optimal long-term care and well-being for individuals with port-wine stains can be achieved.
References:
- R IJM, Arumugam Venkatachalam Sargurunathan E, Gowda Venkatesha RR, Rajaram Mohan K, Fenn SM. Port-wine stains and intraoral hemangiomas: A case series. Cureus. 2024;16(6):1–10.
- Minkis K, Geronemus RG, Hale EK. Port wine stain progression: a potential consequence of delayed and inadequate treatment?. Lasers Surg Med. 2009;41(6):423-6.
- Wolff K, Johnson RA, Saavedra AP. Fitzpatrick dermatology flashcard. New York: Mc Graw Hill Education. 2014. p.70.
- Siskawati Y. Port-wine stain treatment with 577-nm laser: Treatment outcomes of superficial versus deep lesions of superficial versus deep lesions. J Gen Proced Dermatol Venereol Indones. 2024;8(2):112–20.
- Orringer JS. Nonablative Laser and Light-Based Therapy: Cosmetic and Medical Indications. In: Kang S, Amagai M, Bruckner A, Enk AH, Margolis DJ, McMichael AJ, Orringer JS, editors.Fitzpatrick’s Dermatology. 9th ed. McGraw-Hill Education; 2019. p.3848–9.
- Wang B, Mei X, Wang Y, et al. Adjuncts to pulsed dye laser for treatment of port wine stains: a literature review. J Cosmet Laser Ther 2021; 23: 209–17.
- Liu L, Li X, Zhao Q, Yang L, Jiang X. Pathogenesis of Port-Wine Stains: Directions for Future Therapies. Int J Mol Sci. 2022;23(20):1–16.
- Wanitphakdeedecha R, Ng JNC, Yan C, Manuskiatti W, Sudhipongpracha T, Jantarakolica T. Quality of life and psychological effects of port-wine stain: A review of literature. Clinical, Cosmetic and Investigational Dermatology. 2021;14:681–90.
- Hagen SL, Grey KR, Korta DZ, Kelly KM. Quality of life in adults with facial port-wine stains. J Am Acad Dermatol. 2017;76(4):695–702.
- Lipińska K, Bień N, Rajczak M, Niedźwiedź M, Kowalski P, Kobusiewicz A, et al. Port-wine stain and its influence on patients’ quality of life and psychosocial issues. Postepy Dermatol Alergol. 2025;42(3):313-9.
